 |
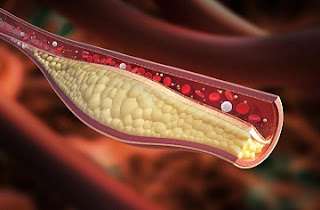
| High cholesterol: Symptoms and causes |
Cholesterol is a waxy substance found
in your blood. Your body needs cholesterol to build healthy cells, but high
levels of cholesterol can increase your risk of heart disease.
With high cholesterol, you can develop
fatty deposits in your blood vessels. Eventually, these deposits grow, making
it difficult for enough blood to flow through your arteries. Sometimes, those
deposits can break suddenly and form a clot that causes a heart attack or
stroke.
High cholesterol can be inherited, but
it's often the result of unhealthy lifestyle choices, which make it preventable
and treatable. A healthy diet, regular exercise, and sometimes medication can
help reduce high cholesterol.
Symptoms
High cholesterol has no symptoms. A
blood test is the only way to detect if you have it.
When to see a doctor
According to the National Heart, Lung, and Blood
Institute (NHLBI), a person's first cholesterol screening should occur between
the ages of 9 and 11 and then be repeated every five years after that.
The NHLBI recommends that cholesterol
screenings occur every one to two years for men ages 45 to 65 and for women ages
55 to 65. People over 65 should receive cholesterol tests annually.
If your test results aren't within desirable ranges, your doctor might recommend more-frequent measurements. Your doctor might also suggest more-frequent tests if you have a family history of high cholesterol, heart disease, or other risk factors, such as diabetes or high blood pressure.
Causes
Cholesterol is carried through your blood, and attached to proteins.
This combination of proteins and cholesterol is called a lipoprotein. There are
different types of cholesterol, based on what the lipoprotein carries. They
are:
Low-density lipoprotein (LDL).
LDL, the "bad" cholesterol, transports cholesterol particles throughout your body. LDL cholesterol builds up in the walls of your arteries, making them hard and narrow.High-density lipoprotein (HDL).
HDL, the "good" cholesterol, picks up excess cholesterol and takes it back to your liver.A lipid profile also typically measures triglycerides, a type of
fat in the blood. Having a high triglyceride level also can increase your risk
of heart disease.
Factors you can control — such as inactivity, obesity, and an
unhealthy diet — contribute to harmful cholesterol and triglyceride levels.
Factors beyond your control might play a role, too. For example, your genetic
makeup might make it more difficult for your body to
remove LDL cholesterol from your blood or break it down in the liver.
Medical conditions that can cause unhealthy cholesterol levels include:
- Chronic kidney disease
- Diabetes
- HIV/AIDS
- Hypothyroidism
- Lupus
Cholesterol levels can also be worsened by some types of
medications you may be taking for other health problems, such as:
- Acne
- Cancer
- High blood pressure
- HIV/AIDS
- Irregular heart rhythms
- Organ transplants
Risk factors
Factors that can increase your risk of
unhealthy cholesterol levels include:
Poor diet.
Eating too much-saturated fat or trans fats can result in unhealthy cholesterol levels. Saturated fats are found in fatty cuts of meat and full-fat dairy products. Trans fats are often found in packaged snacks or desserts.Obesity.
Having a body mass index (BMI) of 30 or greater puts you at risk of high cholesterol.Lack of exercise.
Exercise helps boost your body's HDL, the "good," cholesterol.Smoking.
Cigarette smoking may lower your level of HDL, the "good," cholesterol.Alcohol.
Drinking too much alcohol can increase your total cholesterol level.Age.
Even young children can have unhealthy cholesterol, but it's much more common in people over 40. As you age, your liver becomes less able to remove LDL cholesterol.
Complications
High cholesterol can cause a dangerous
accumulation of cholesterol and other deposits on the walls of your arteries
(atherosclerosis). These deposits (plaques) can reduce blood flow through your
arteries, which can cause complications, such as:
Chest pain.
If the arteries that supply your heart with blood (coronary arteries) are affected, you might have chest pain (angina) and other symptoms of coronary artery disease.Heart attack.
If plaques tear or rupture, a blood clot can form at the plaque-rupture site — blocking the flow of blood or breaking free and plugging an artery downstream. If blood flow to part of your heart stops, you'll have a heart attack.Stroke.
Similar to a heart attack, a stroke occurs when a blood clot blocks blood flow to part of your brain.
Prevention
The same heart-healthy lifestyle
changes that can lower your cholesterol can help prevent you from having high
cholesterol in the first place. To help prevent high cholesterol, you can:
- Eat a
low-salt diet that emphasizes fruits, vegetables, and whole grains
- Limit
the number of animal fats and use good fats in moderation
- Lose
extra pounds and maintain a healthy weight
- Quit
smoking
- Exercise
on most days of the week for at least 30 minutes
- Drink
alcohol in moderation, if at all
- Manage
stress
Diagnosis
A blood test to check cholesterol
levels — called a lipid panel or lipid profile — typically reports:
- Total
cholesterol
- LDL cholesterol
- HDL cholesterol
- Triglycerides
— a type of fat in the blood
Generally, you're required to fast,
consuming no food or liquids other than water, for nine to 12 hours before the
test. Some cholesterol tests don't require fasting, so follow your doctor's
instructions.
Interpreting the numbers
In the United States, cholesterol
levels are measured in milligrams (mg) of cholesterol per deciliter (dL) of
blood. In Canada and many European countries, cholesterol levels are measured
in millimoles per liter (mmol/L). To interpret your test results, use these general
guidelines.
Children and cholesterol testing
For most children, the National Heart,
Lung, and Blood Institute recommends one cholesterol screening test between the
ages of 9 and 11, and then be repeated every five years after that.
If your child has a family history of
early-onset heart disease or a personal history of obesity or diabetes, your
doctor might recommend earlier or more-frequent cholesterol testing.
Treatment
Lifestyle changes such as exercising
and eating a healthy diet are the first line of defense against high
cholesterol. But, if you've made these significant lifestyle changes and your
cholesterol levels remain high, your doctor might recommend medication.
The choice of or combination of medications depends on various factors, including your personal risk factors, age, health, and possible drug side effects. Common choices
include:
Statins.
Statins block a substance your liver needs to make cholesterol. This causes your liver to remove cholesterol from your blood. Choices include atorvastatin (Lipitor), fluvastatin (Lescol), lovastatin (Altoprev), pitavastatin (Livalo), pravastatin (Pravachol), rosuvastatin (Crestor) and simvastatin (Zocor).Cholesterol absorption inhibitors.
Your small intestine absorbs the cholesterol from your diet and releases it into your bloodstream. The drug ezetimibe (Zetia) helps reduce blood cholesterol by limiting the absorption of dietary cholesterol. Ezetimibe can be used with a statin drug.Bempedoic acid.
This newer drug works in much the same way as statins but is less likely to cause muscle pain. Adding bempedoic acid (Nexletol) to a maximum statin dosage can help lower LDL significantly. A combination pill containing both bempedoic acid and ezetimibe (Nexlizet) also is available.-
Bile-acid-binding resins.
Your
liver uses cholesterol to make bile acids, a substance needed for
digestion. The medications cholestyramine (Prevalite), colesevelam
(Welchol), and colestipol (Colestid) lower cholesterol indirectly by
binding to bile acids. This prompts your liver to use excess cholesterol
to make more bile acids, which reduces the level of cholesterol in your
blood.PCSK9 inhibitors.
These drugs can help the liver absorb more LDL cholesterol, which lowers the amount of cholesterol circulating in your blood. Alirocumab (Praluent) and evolocumab (Repatha) might be used for people with a genetic condition that causes very high levels of LDL or in people with a history of coronary disease who are intolerant to statins or other cholesterol medications. They are injected under the skin every few weeks and are expensive.Medications for high triglycerides
If you also have high triglycerides,
your doctor might prescribe:
Fibrates.
The medications fenofibrate (Tricor, Fenoglide, others) and gemfibrozil (Lopid) reduce your liver's production of very-low-density lipoprotein (VLDL) cholesterol and speed the removal of triglycerides from your blood. VLDL cholesterol contains mostly triglycerides. Using fibrates with a statin can increase the risk of statin side effects.Niacin.
Niacin limits your liver's ability to produce LDL and VLDL cholesterol. But niacin doesn't provide additional benefits over statins. Niacin has also been linked to liver damage and strokes, so most doctors now recommend it only for people who can't take statins.Omega-3 fatty acid supplements.
Omega-3 fatty acid supplements can help lower your triglycerides. They are available by prescription or over-the-counter. If you choose to take over-the-counter supplements, get your doctor's OK. Omega-3 fatty acid supplements could affect other medications you're taking.Tolerance varies
Tolerance of medications varies from
person to person. The common side effects of statins are muscle pains and
muscle damage, reversible memory loss and confusion, and elevated blood sugar.
If you decide to take cholesterol medication, your doctor might recommend liver
function tests to monitor the medication's effect on your liver.
Children and cholesterol treatment
Diet and exercise are the best initial
treatment for children aged 2 and older who have high cholesterol or who are
obese. Children aged 10 and older who have extremely high cholesterol levels
might be prescribed cholesterol-lowering drugs, such as statins.
Lifestyle and home remedies
Lifestyle changes are essential to
improve your cholesterol levels.
- Lose extra pounds. Losing
weight can help lower cholesterol.
- Eat a heart-healthy diet. Focus
on plant-based foods, including fruits, vegetables, and whole grains. Limit
saturated fats and trans fats. Monounsaturated fat, found in olive and
canola oils, is a healthier option. Avocados, nuts, and oily fish are other
sources of healthy fat.
- Exercise regularly. With
your doctor's OK, work up to at least 30 minutes of moderate-intensity
exercise five times a week.
- Don't smoke. If you
smoke, find a way to quit.
( Keywords )


Post a Comment